The Bone Graft Question: When You Actually Need One for Implants (and When You Don’t)
If you’ve started researching dental implants, you’ve probably run into the phrase “bone graft” and felt your stomach drop a little. It sounds invasive. It sounds expensive. And it sounds like one more hurdle between you and a replaced tooth.
Here’s what most implant websites won’t tell you directly: not everyone needs a bone graft. Some patients have plenty of bone and can proceed straight to implant placement. Others genuinely need grafting, and skipping it would compromise the result. And a smaller group falls somewhere in between, where clinical judgment (not a sales quota) should determine the path forward.
Let’s sort through what bone grafting actually is, who needs it, who doesn’t, and how to tell if your provider is recommending it for the right reasons.
What a Bone Graft Actually Does
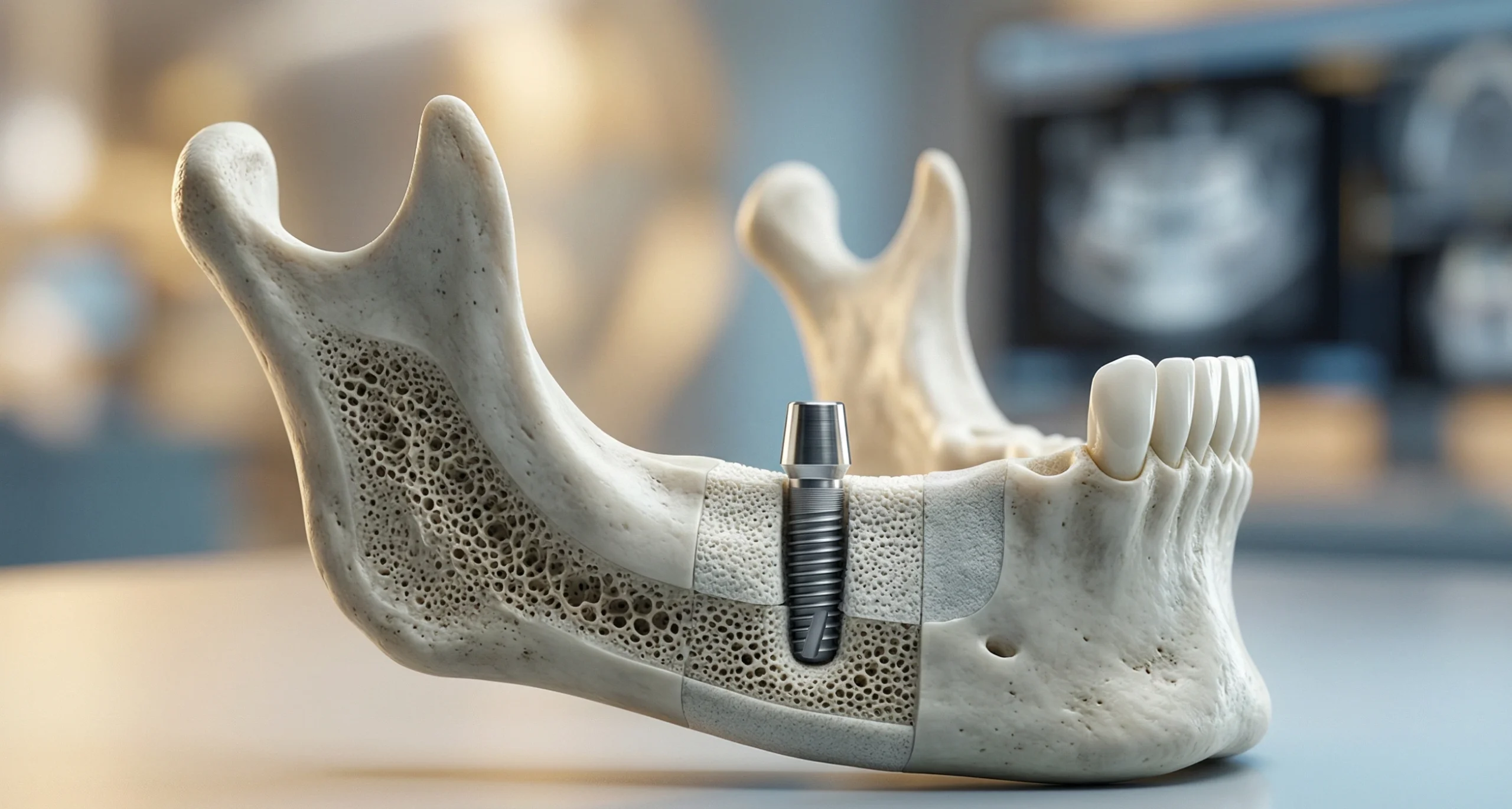
A bone graft adds volume to your jawbone in areas where it has thinned or deteriorated. The graft material acts as a scaffold that your body gradually replaces with new, natural bone over several months.
Think of it like patching a wall before hanging a heavy shelf. The implant is the shelf. The graft rebuilds the wall so it can hold the weight.
Graft material can come from several sources:
Autograft: Bone harvested from another area of your own body (often the chin or back of the jaw). This is the gold standard for biological compatibility, but it requires a second surgical site.
Allograft: Donor bone from a tissue bank, processed and sterilized for safe use. This is the most common type used in dental implant grafting.
Xenograft: Bone derived from animal sources (typically bovine), processed to remove organic material and leave the mineral structure.
Synthetic graft: Lab-made materials designed to mimic bone structure and encourage new growth.
Your provider will choose the graft type based on the size of the defect, the location in your jaw, and your health history.
Why Bone Loss Happens in the First Place
Your jawbone stays healthy because your teeth stimulate it. Every time you chew, the roots of your teeth transfer force into the bone, which signals your body to keep that bone strong and dense.
When a tooth is removed or falls out, that stimulation stops. The bone in that area begins to resorb (shrink) within weeks. After a year without a tooth, you can lose 25% of the bone width in that area. After several years, the loss is significant.
This is why timing matters so much with implants. The sooner you place an implant after losing a tooth, the less bone you lose and the less likely you are to need a graft.
Other factors that accelerate bone loss include:
- Long-term denture wear (dentures press on bone without stimulating it)
- Gum disease that has damaged the bone around teeth
- Infections or abscesses that erode bone tissue
- Certain medications that affect bone metabolism
- Aging, which naturally reduces bone density
Who Actually Needs a Bone Graft
Bone grafting is necessary when there isn’t enough bone to safely and securely hold an implant post. The implant needs a minimum amount of bone height, width, and density to integrate properly and support a crown.
You likely need a graft if:
You lost a tooth more than a year ago and haven’t replaced it. The longer the gap, the more bone loss. If a 3D scan shows the ridge has narrowed or shortened significantly, grafting rebuilds what’s been lost.
You had gum disease (periodontitis) that destroyed bone. Periodontal disease doesn’t just affect your gums. Advanced cases eat away at the bone that holds your teeth in place. Even after the disease is treated, the bone doesn’t grow back on its own.
You need an implant in the upper back jaw near the sinus. The maxillary sinus sits directly above the roots of your upper molars. When those teeth are lost, the sinus can expand downward into the space, leaving very little bone for an implant. A sinus lift (a specific type of bone graft) raises the sinus floor and adds bone beneath it.
Your 3D scan shows insufficient bone volume. This is the definitive answer. A CBCT scan measures exactly how much bone you have in every dimension. If the numbers fall below the minimums for safe implant placement, grafting is the path forward.
Who Probably Doesn’t Need One
Not every implant case requires grafting, and it’s worth knowing when it’s genuinely unnecessary.
You lost the tooth recently and the bone is intact. If you’re getting an implant within a few months of extraction, especially if the tooth was removed carefully and the socket was preserved, you may have plenty of bone.
Your extraction included socket preservation. Some providers place graft material into the extraction socket at the time of removal. This is called socket preservation or ridge preservation, and it maintains bone volume so a graft isn’t needed later.
You have naturally thick, dense bone. Some people just have more bone to work with. Younger patients, patients with good overall bone health, and patients with a thick jaw ridge often have enough volume for implants without additional grafting.
You’re getting an implant in the lower front jaw. This area of the mouth tends to retain bone better than other regions, even after tooth loss.
The Gray Area: When It’s a Judgment Call
Many cases aren’t clear-cut. The bone might be borderline, where it could support an implant but with less margin for error. Or the bone might be adequate in one dimension but thin in another.
In these situations, the decision to graft or not depends on the provider’s experience and philosophy.
A conservative provider might recommend grafting to maximize long-term success, even if the implant could technically be placed without it. That’s a defensible approach.
An experienced provider with high case volume might feel confident placing the implant without grafting, using a slightly narrower implant or a different angle to work with the available bone. That’s also defensible, as long as the decision is based on 3D data and not guesswork.
What’s not defensible is recommending a graft without a 3D scan. If your provider suggests bone grafting based only on a 2D X-ray or a visual exam, that’s incomplete information driving a surgical decision.
How to Know if Your Provider Is Recommending It for the Right Reasons
Ask these questions:
“Can you show me the scan that shows where the bone is insufficient?” A provider with a CBCT scan should be able to point to the exact area of concern and explain why grafting is needed. If they can’t show you the data, push back.
“What happens if we skip the graft?” A transparent provider will explain the specific risks: implant instability, failure to integrate, compromised crown placement. If the answer is vague or fear-based without specifics, that’s a concern.
“Could a different implant size or angle work without grafting?” Sometimes a narrower or shorter implant, placed at a slightly different angle, can succeed without a graft. Not every provider considers this option, but it’s worth asking.
“How long does the graft add to the overall timeline?” A bone graft typically needs three to six months to mature before an implant can be placed. If your provider glosses over this timeline, they may not be giving you the full picture.
What Grafting Costs
Bone grafting costs vary based on the type and extent of the procedure:
- Socket preservation at the time of extraction: $300 to $800
- Minor ridge augmentation: $500 to $1,500
- Major block graft or sinus lift: $1,500 to $3,500
These costs are on top of the implant itself. Your provider should include grafting in the total treatment estimate so there are no surprises. For a complete breakdown of what implant treatment costs in Chicago, including grafting, see our pricing guide.
The Takeaway
Bone grafting isn’t something to fear. It’s a routine, well-documented procedure that has been performed in dentistry for decades. When it’s genuinely needed, it creates the foundation that makes your implant successful for years to come.
But it shouldn’t be assumed as a default for every implant case. And it shouldn’t be recommended without 3D imaging that shows exactly where and why the bone is insufficient.
The best way to get a clear answer is to see a provider who plans implant cases with precision, not guesswork. At Bite Club, we use CBCT imaging on every implant case and walk you through the scan so you can see exactly what we see.
If you’ve been told you need a bone graft and want a second opinion, or if you’re starting from scratch and want to know what your implant case actually requires, reach out to schedule a consultation. We’ll give you a straight answer based on your specific anatomy.
